| Table of Contents |  |
|
Original Article
| ||||||
| Factors associated with knowledge and attitude to the use of dental floss at some private and public dental clinics in Lagos State | ||||||
| Oyapero A.1, Owoturo E.O.2 | ||||||
|
1Department of Preventive Dentistry, Lagos State University Teaching Hospital, Ikeja, Lagos Nigeria.
2Department of Restorative Dentistry, Lagos State University Teaching Hospital, Ikeja, Lagos Nigeria. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Oyapero A, Owoturo EO. Factors associated with knowledge and attitude to the use of dental floss at some private and public dental clinics in Lagos State. Edorium J Dent 2016;3:12–20. |
|
Abstract
|
|
Aims:
Dental caries and periodontal diseases which are the two most prevalent oral diseases are dental biofilm dependent. This effect of dental plaque is particularly evident in the interproximal region. The aim of this study was to determine the factors that are associated with knowledge and positive attitude towards the use of dental floss at the Lagos State University Teaching Hospital, Ikeja, (LASUTH) and two private dental clinics in Ikeja and Magodo, Lagos State.
Methods: This prospective descriptive study was conducted at the oral diagnosis clinic of LASUTH and at two private dental clinics in Lagos State. A structured interviewer administered questionnaire was used to obtain information on socio-demographic items and on the participant's perception regarding gum inflammation, their oral hygiene practices and their knowledge, attitude and practices related to flossing. Results: The study population included dental patients aged 22–68 years. Majority of the respondents in this present study had poor knowledge and attitude on the use of dental floss. Respondents attending the private clinics had significantly better knowledge on the practice of oral hygiene and the use of dental floss (p = 0.000) and they also had a more positive attitude even though the association was not significant. (p = 0.364) The study participants that had a good knowledge and positive attitude on dental floss usage and oral hygiene had lower mean OHI-S, GI and DMFT scores even though the association was not significant. Conclusion: This study demonstrated a poor level of knowledge and attitude to the use of dental floss among the respondents. Oral health care professionals should spend adequate time to educate their patients on the benefits of interproximal cleaning especially floss usage. They should also enhance the self-efficacy and knowledge of their patients about the benefits of interdental hygiene. | |
|
Keywords:
Dental flossing, Dental plaque, Hygiene, Oral
| |
|
Introduction
| ||||||
|
Dental caries and periodontal diseases which are the two most prevalent oral diseases are dental biofilm dependent. A wide variation in oral biofilm formation between different areas is the mouth is known to exist. This effect of dental plaque is particularly evident in the interproximal region. Due to the size and shape of the interproximal region, it constitutes an ecological niche in which an undisturbed biofilm can form. Oral microorganisms and food products easily become attached interproximally and access by saliva to this site is limited. Diseases of periodontal tissues are the result of an accumulation of plaque and calculus, and the proliferation of pathogenic organisms subgingivally within the sulcus, especially interproximally. Similarly, most caries-prone areas of the teeth are the interproximal surfaces, the fissures and the gingival third of the smooth surfaces which are associated with undisturbed plaque accumulation [1]. Plaque at interproximal sites has been reported to be more acidogenic than in other areas of the mouth [2]. An increased prevalence of interproximal caries has been found in relation to high caries risk [3] and interproximal surfaces are regarded as especially high-risk sites for caries in individuals with high sugar consumption. Plaque control aims to prevent the development of dental caries and periodontal disease and the appropriate use of a toothbrush has been the most frequently recommended tool for oral hygiene. The toothbrush is effective in the removal of plaque deposits on the occlusal, buccal/labial and the lingual/palatal surfaces of the teeth. It however has a very limited role in the removal of interproximal deposits of plaque. A recent systematic review of available evidence has shown that tooth brushing alone plays an inadequate role in caries prevention, [4] due to poor access to the proximal surfaces of teeth. Hence, interproximal cleaning is recommended to further help in preventing both dental caries and periodontal disease [5]. Since the interproximal area is usually the site of onset of gingival inflammation, interproximal plaque control should be an essential component of oral hygiene measures. Daily mechanical removal of supragingival oral biofilm with a toothbrush and interdental cleaning aids is thus indispensable for proper plaque control [6] [7]. The most common interdental cleaning devices are dental floss, interdental brushes in various sizes, and triangular wood sticks in different widths. Dental flossing is the most common method of interproximal cleaning recommended by dentists and utilized by patients [8]. Flossing is a preventative health behavior, which removes plaque from areas that brushing cannot reach, [9] thereby preventing cavities and gum disease [10]. Flossing has been shown to be associated with greater plaque reduction than brushing alone [11]. Flossing is most effective when performed daily, preferably in the evening, to prevent bacteria build-up when asleep [12]. Several studies have shown the usefulness of regular dental flossing for removing interdental plaque and preventing calculus formation [13][14]. The daily use of dental floss once a day for six weeks also resulted in a reduction in both plaque scores and gingivitis [15]. The evidence of effectiveness of flossing on caries prevention is however not very strong [16]. While no effect on the caries rate was found after supervised daily flossing for three year, a caries-prevention effect was found in a group of 10–11 years old children using fluoride-free dental floss more than every second day for two years [17] . There is a need to explore the knowledge and attitude of dental patients to the use of dental floss due to the dearth of publications exploring the use of interdental cleaning devices in Nigeria. The aim of this study was to determine the factors that are associated with knowledge and attitude to the use of dental floss at the Lagos State University Teaching Hospital, Ikeja, (LASUTH) and two private dental clinics in Ikeja and Magodo, Lagos State. | ||||||
|
Materials and Methods
| ||||||
|
This prospective descriptive study was conducted at the Oral Diagnosis Clinic of the Lagos State University Teaching Hospital, Ikeja, Lagos (LASUTH) and at two private dental clinics in Lagos State. Sample selection Sample size Study Setting and location. Inclusion and Exclusion criteria Data collection Knowledge regarding gum inflammation and dental floss usage Attitudes regarding health beliefs and barriers limiting use of dental floss Intraoral Examination Oral hygiene index-simplified (OHI-S) [20] was used to assess oral cleanliness by estimating the tooth surface covered with debris or calculus. The two components: Simplified debris index (DI) and Simplified calculus index (CI) were combined for the OHI-S score. After determining the simplified debris index and simplified calculus index scores, the total score was divided by the number of surfaces examined to obtain a DI and CI values ranging from 0–3. The simplified oral hygienic index score was obtained by combining the DI and CI with a value range from 0–6. Community periodontal index of treatment needs (CPITN) was assessed with W.H.O recommended probe, CPITN-C probe which is designed for gentle manipulation of the sensitive soft tissues around the teeth. The molars were examined in pairs and the highest score was recorded. The six sextant scores were recorded as the CPITN scores of the participant. Data analysis | ||||||
|
Results | ||||||
|
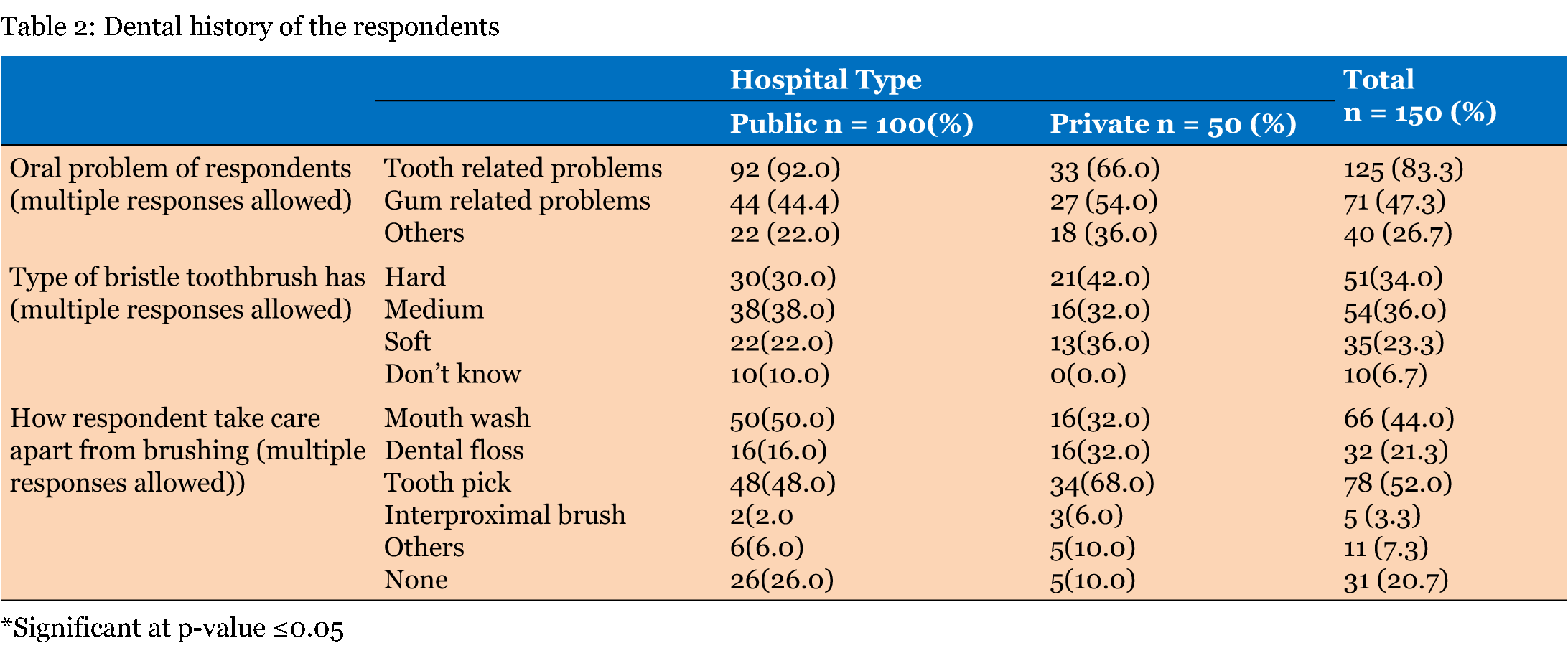
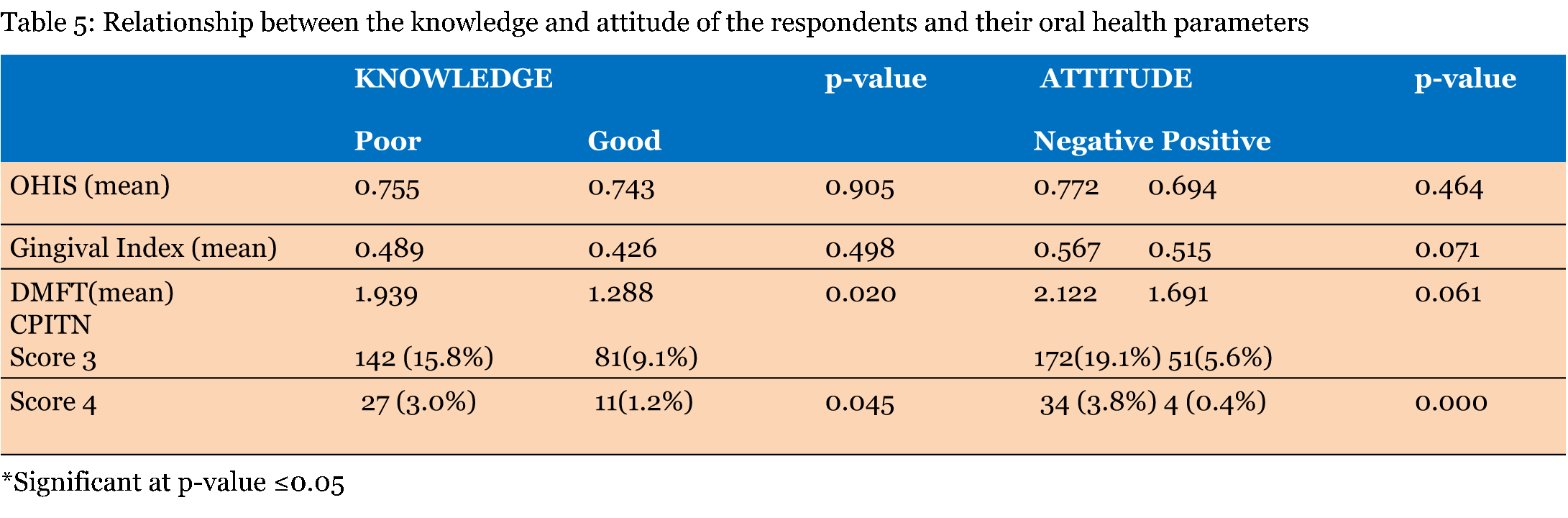
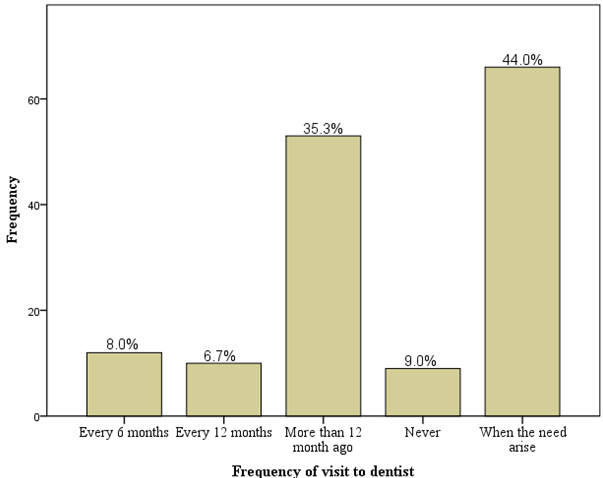
The study population included dental patients aged 22–68 years. The gender, educational level, age distribution and income level of the respondents based on the type of dental clinic attended is given in Table 1. Females, those aged 41–50 years, Tertiary educated, and those earning more than 200,000 naira monthly were significantly more likely to attend a private dental clinic. Table 2 describes the pattern of dental conditions in patients presenting in the public and at the private dental clinics. Majority of the respondents had tooth related pathologies while 34% of the respondents routinely used hard bristle toothbrushes. Toothpick (52%) was the most common brushing adjunct that the participants used while interdental brushes were the least common (3.3%). Table 3 illustrates the relationship between the knowledge and attitude towards dental floss usage among patients attending public and private dental clinics. Respondents attending the private clinics had significantly better knowledge on the practice of oral hygiene and the use of dental floss (p = 0.000) and they also had a more positive attitude even though the association was not significant (p = 0.364). Table 4 illustrates the relationship between the knowledge and attitude of the participants towards dental floss usage and their socio-demographic variables. Females and tertiary educated respondents had significantly better knowledge on oral hygiene and dental floss use. Similarly, females, respondents aged 41–50 years and those with a monthly income above 200,000 naira had a significantly more positive attitude to dental floss use. Table 5 gives the relationship between the knowledge and attitude of the respondents and their periodontal and dental parameters. The study participants that had a good knowledge and positive attitude on dental floss usage and oral hygiene had lower mean OHI-S, GI and DMFT scores even though the association was not significant. Similarly, out of the 900 sextants examined in the 150 respondents, only 92 (10.3%) of those that had good knowledge had CPITN scores of 3 and 4. Table 6 tells the association between the mean knowledge and attitude scores of the respondents and their socio-demographic variables. Respondents that attended private dental clinics, those aged between 41–50 years, tertiary educated respondents and those that earned above 200,000 naira monthly had significantly higher mean knowledge scores. Figure 1 displays the frequency of visits by the respondents to the dentist. Forty-four percent of them only visit when the need arises while only 14.7 visit every 6–12 months. | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
In this study, almost an equal number of male and female respondents were seen at the public hospital while females were significantly predominant in the private hospital respondents. A greater percentage of the public hospital respondents were aged between 21–30 years old while the private hospital respondents were predominantly aged between 41–50 years old. All the respondents attending the private dental clinic had tertiary education and a greater percentage of them earned above 200,000 naira monthly (Table 1). Obtaining of dental care services is related to the ability to access oral health resources [21]. Socio-demographic factors such as education, income, social status and location affect the use of oral health services and have a collective impact on oral health and oral health disorders [16]. In Nigeria, patients in the lower socio-demographic groups tend to access public health facilities while private dental clinics, which usually located in the metropolis are usually utilized by the wealthy. Dental care is significantly cheaper in the public sector in Nigeria and the majority of the population still has limited financial access to oral health care because the main method of financing oral health care services remains out-of pocket payments [22]. The pattern of dental attendance by the respondents was based on emergency demand rather than for preventive or regular care. Less than 15% of the respondents attended the dental clinic at least once a year (Figure 1). Previous research has shown that patients in the Sub-Saharan Region of Africa have a low level of utilization of dental services and that they seek oral health care mainly for curative rather than preventive services [23]. Dental caries and periodontal diseases were the prevalent oral diseases seen in these groups of respondents (Table 2). These dental conditions are primarily plaque related conditions in spite of the role that diet, systemic conditions and other oral habits have in the aetiology of these conditions. The regular removal of dental plaque biofilm, which contains the bacteria responsible for caries formation and for the aetiology of gingivitis and periodontitis, is thus indispensable to dental health [24]. Tooth brushing was the most common oral hygiene procedure performed by patients. Effective brushing remains the most obvious way of maintaining low levels of plaque and good gingival health. Most of the respondents however did not adhere to the use of the right type of toothbrush. Interproximal cleaning is also important, since toothbrush alone is ineffective in reaching the areas that carry a high risk of developing periodontal disease. Toothpicks were the most common type of interdental cleaning aid used by the respondents. Less than 20% of the respondents utilized interdental brushes or dental floss for interdental cleaning (Table 2). Most individuals are conscious of the need for regular oral hygiene maintenance. However despite recommendations by dental professionals, the rates of flossing among individuals are consistently lower than those of tooth brushing [25]. Although it is universally recognized by dentists that interproximal cleansing is essential for controlling periodontal disease, compliance with floss usage is generally low [26]. Majority of the respondents in this present study had poor knowledge on the use of dental floss even though respondents from the private clinics had significantly better responses than those in the public hospitals (Table 3). A similar observation was noted in the attitude of the respondents. Females and tertiary educated respondents had significantly better knowledge on oral hygiene and dental floss use. Likewise, Females, respondents aged 41–50 years and those with a monthly income above 200,000 naira had a significantly more positive attitude to dental floss use (Table 4) and (Table 5) Oral self-care behaviors have been observed to be better among higher-educated persons. The additional cost to be incurred in the purchase of dental floss may be a barrier to the purchase of dental floss in indigent patients. Females have also been observed to be more motivated with regard to oral hygiene practices and thus brush their teeth more frequently than males [27]. A survey of 186 Finnish university students also revealed that 40% of females and 25% of males reported using dental floss but that only 2% of all students flossed daily [28]. Factors such as time wasting and the need for manual dexterity have been given as reasons for insufficient interproximal cleaning [29]. Educating and motivating patients on interdental cleaning should adequately focus on males who tend to have a higher prevalence of periodontal disease. The study participants that had a good knowledge and positive attitude on dental floss usage and oral hygiene had lower mean OHI-S, GI and DMFT scores even though the association was not significant (Table 5). Similarly, out of the 900 sextants examined in the 150 respondents, only 92 (10.3%) of those that had good knowledge had CPITN scores of 3 and 4 (Table 5). Diligent flossing and brushing must supplement professional plaque removal for healthy teeth because plaque begins to form within two hours of the time it has been removed, and research has shown that allowing plaque to accumulate on clean teeth surfaces for 2 to 3 weeks can cause gingivitis [16]. Thus, ongoing home dental care is essential since it has been found that thorough daily plaque removal decreases the risk of gingivitis and periodontitis. | ||||||
|
Conclusion
| ||||||
|
This study demonstrated a poor level of knowledge and attitude to the use of dental floss among the respondents. There is a well-documented body of evidence supporting the effective use of dental floss on interproximal cleaning. Oral health care professionals should spend adequate time to educate their patients on the benefits of interproximal cleaning especially floss usage. They should consider interventions that reward positive behavior and foster intrinsic motivation. They should also enhance the self-efficacy and knowledge of their patients about the benefits of interdental hygiene. A major limitation of this study is the cross sectional nature of the study design which will not permit conclusive inferences to be made from its observations. Similarly, some of the responses elicited from the participants could be subject to recall and "social desirability" bias. A longitudinal study may hence help to validate the significant findings of this research. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Oyapero A. – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Owoturo E.O. – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Oyapero A. et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|